Take a look at our Q&A session with Sonia Chopra, DDS, of Ballantyne Endodontics to get the answers to your root canal questions!
Ask the Endodontist: Dr. Sonia Chopra
Question: What are the main root canal symptoms that patients should be aware of?
Answer: Patients can experience a number of root canal symptoms that cause discomfort and pain. Most of the time, though, when I see patients needing a root canal, they have one of three symptoms:
- Pain to cold
- Pain to heat
- Pain to biting
Some patients even experience a combination of the three. It’s important if you’re experiencing root canal pain or discomfort that you reach out to a dental provider immediately to determine next steps.
Question: What are ways to help avoid the need for a root canal treatment?
Answer: Prevention is key! You want to avoid needing a root canal in general. A lot of people are scared of the dentist or put off dental appointments, but the best way to keep your teeth healthy is regular checkups.
When you think about it, you have 32 chances of needing a root canal—and your six-month checkups are a great opportunity to prevent that from happening. Keep seeing your dentist to catch issues early, as it’s much more effective and cheaper to do a simple filling versus needing a root canal and a crown afterwards.
Question: What should patients keep in mind when they’re deciding on how to address a root canal issue?

Answer: There’s a lot of non-factual information on the internet about root canals, and some people have negative beliefs about them. From my own personal experience after having two root canals, though, I can say that they saved me from excruciating pain. They got rid of the disease while allowing me to save my tooth and its natural function. People are typically in pain because they need a root canal—but what they don't realize is the root canal is the alleviator of the pain.
When a patient needs a root canal, he or she should work with a dental provider to:
- Make sure that the tooth warrants the root canal
- Make sure that the tooth is savable and that there's enough tooth structure in order to save the tooth
- Decide between doing the root canal non-surgically or surgically
If there are a lot of restorations in the way, sometimes you have to take a surgical approach to treat the tooth. Every tooth situation is unique, though, so your dentist or endodontist will need to understand the underlying factors before deciding on the treatment option.
Additionally, everyone really should prioritize saving their teeth when they can; there are definitely a number of hidden values that people don’t really appreciate. I like to compare teeth to your fingers—you have ten fingers, and you’d do anything to save them, so why not do the same for your teeth? They do so much for us as the gateway to our body and with healthy teeth, people are better suited for a long, healthy life.
“If you can save your tooth, it will provide such a benefit to your overall health—and even your longevity.”
Question: What is the difference between a dentist and an endodontist and what are the advantages and disadvantages of each?
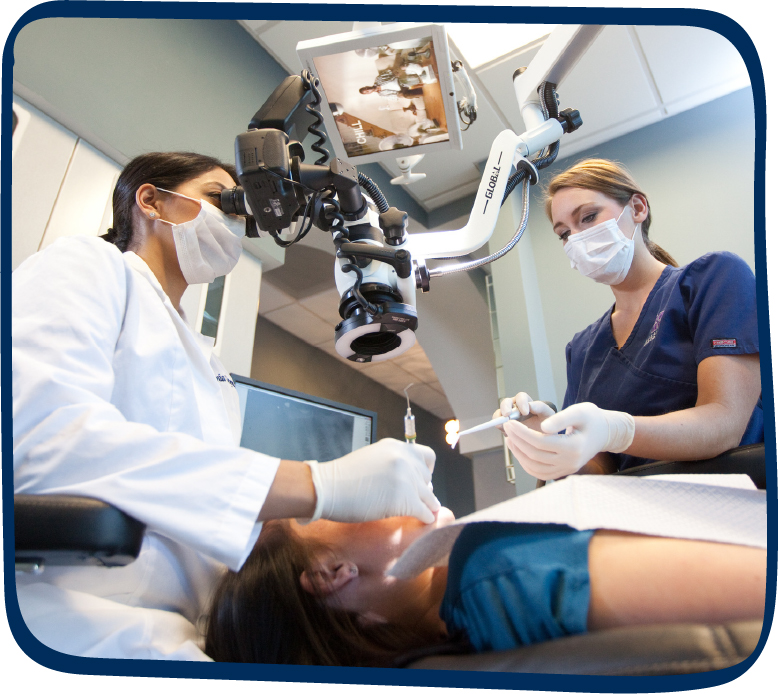 Answer: A general dentist is one who does all; as a provider, they can perform a number of procedures in-house. Patients can be apprehensive to meet other clinicians, so it’s really important for general dentists to be able to perform basic root canals—but they also need to set boundaries to know which type of root canal they want to complete versus what is better suited for a specialist.
Answer: A general dentist is one who does all; as a provider, they can perform a number of procedures in-house. Patients can be apprehensive to meet other clinicians, so it’s really important for general dentists to be able to perform basic root canals—but they also need to set boundaries to know which type of root canal they want to complete versus what is better suited for a specialist.
If a case is really difficult or requires a different level of skill, a dentist will refer to an endodontist, who is a specialist of root canals. Endodontists go to school for an extra two to three years—and root canals are their primary work. An endodontist may do root canals up to ten times a day, whereas a general dentist may only do one a week. People don't always realize how specialized dentistry is, and there are so many little details in endodontics that are important to getting the procedure right.
Question: What made you choose to become an endodontist?
Answer: I actually picked being an endodontist because of my own root canal experience.
When I was 17 years old, I had a toothache that nobody could diagnose, and they didn't know where it was coming from. I ended up seeing about seven different doctors, and they were all perplexed at what the source of my pain was. I was not referred to an endodontist initially; I was actually referred to an oral surgeon who was instructed to extract my tooth. When the anesthesia wore off, though, my toothache was still there; I still had the same pain because they misdiagnosed which tooth it was coming from, and they pulled out the wrong one.
I was finally referred to an endodontist, and he changed my life. He walked me through what was happening to my tooth and helped me understand the whole disease process and what he was doing. He explained the root canal step by step, and I was so impressed by the whole appointment. Afterwards when my anesthesia wore off, I didn't have pain, and I finally felt like myself again.
Being able to experience that and live that helps me understand what my patients go through—and it continues to drive my passion for endodontics.
Question: What can occur if patients delay treatment after their dentist informs them that they need a root canal?
Answer: If a patient delays treatment, the most common thing that happens is that the tooth nerve will die, which can be painful for some. Ultimately, though, when the nerve dies, it can cause an adverse effect to your mouth. Your body doesn’t like the bacteria that killed the nerve, and it will respond by having the bone around your tooth start to pull away from the tooth. This can start bone resorption, and it actually creates a crater in the bone. After that, you can abscess, which will cause swelling or some level of pain or discomfort.
In general, it’s always better to not delay treatment and instead seek care immediately. This will help avoid further complications—and alleviate persistent root canal pain.
For more insights from Dr. Chopra, be sure to check out Tooth Wisdom: The Empowered Patient’s Guide to Saving Your Smile.

Question: For patients who have completed a root canal treatment, what are common symptoms that they could experience afterwards?
Answer: I tell my patients that they're going to be pretty sore if they bite or chew on the tooth for about three to seven days. As long as the soreness is starting to improve after about the third day, they’re heading in the right direction. I recommend keeping food a little bit soft so you don’t startle yourself by biting down on something too hard. Usually, just taking ibuprofen can manage pain and keep the discomfort to a minimum.
 Some patients, though, will swell no matter what just because of how they heal, and I remind those patients that their bodies just need a little extra help and maybe some antibiotics. If they do have postoperative swelling—which can start between one to three days after the procedure—that can be totally normal, and they just need to work with us to determine what they need for optimal recovery.
Some patients, though, will swell no matter what just because of how they heal, and I remind those patients that their bodies just need a little extra help and maybe some antibiotics. If they do have postoperative swelling—which can start between one to three days after the procedure—that can be totally normal, and they just need to work with us to determine what they need for optimal recovery.
We just like to ensure that patients understand anything that can occur during recovery so that they know what to expect—and aren’t startled by any symptoms.
Question: How can patients support long-term success of their treated tooth? What do you advise to your patients?
Answer: If there’s not a crown on the tooth already, it's really important that they get a crown on the tooth. A crown is hugely helpful for structural reasons, as it prevents any cracks from getting bigger, and it provides support to prevent the tooth from splitting and needing to be extracted. The crown additionally creates a seal so that no new bacteria can get in after the tooth has been disinfected.
Getting a crown in a timely manner—which is typically about two weeks after the root canal is done—is really crucial for long-term success.
For more recommendations on how to take care of your tooth after a root canal treatment, download Root Canal Recovery: Taking Care of Your Tooth After Treatment!
Question: Have you noticed any postoperative recovery difference now that you've integrated the GentleWave® Procedure into your practice?
Answer: 100%; it’s night and day in what my patients feel. I like to do my own postoperative calls, and my patients are describing a more comfortable recovery; I no longer prescribe pain medicine, and I rarely prescribe antibiotics.
Personally, I’ve had both a traditional root canal and a GentleWave Procedure root canal. When I had the traditional root canal, afterwards I was pretty sore for a bit, and my soreness didn't really ever go away. I had my traditional root canal before I had the GentleWave Procedure in my practice, and my tooth still felt a little uncomfortable when the treatment was over. I decided to redo the root canal and see what the GentleWave Procedure was like—and it was absolutely painless.
“I felt like the healing was a lot easier, and I wasn't as sore; I definitely had an easier recovery with the GentleWave® Procedure.”
Question: What is the biggest benefit of the GentleWave Procedure for your patients?
Answer: I’d say one of the biggest benefits is the ability to shift my treatment model from two visits to one visit. A lot of my cases previously involved having patients schedule two appointments—which cut into their everyday lives.
With the GentleWave Procedure, I can typically limit their treatment to one visit. Some cases are too infected and still require a second visit; however, I’d say 90% of what I do now is done in one visit, creating a huge benefit to the patients.
“With the GentleWave Procedure, I can pretty much do everything in one visit, helping expedite treatment times.”
Additionally, with the GentleWave Procedure, patients get to experience decreased postoperative pain and that coupled with the decreased number of visits has created a big change in our patient care.
Question: Is there any additional information that would be beneficial for patients to know?

Answer: Patients know their bodies best, and they really should be an advocate for themselves. Take the time to evaluate if you need to seek out more answers or find a specialist to help you get those answers. It’s important that patients start doing their own research and pick a provider that works for them. When I see a new patient, I want them to interview me to make sure I’m the right provider for them; I think that’s super important.
In general, your tooth should feel good—you should be able to chew on it with no problem. If you're questioning that or if you're questioning your care, though, it’s crucial to seek out more answers.
Looking to Experience the GentleWave® Procedure?
If you’re in need of a root canal and are interested in the GentleWave Procedure, schedule a consultation today by finding a nearby GentleWave Doctor!
